Psoriatic arthritis (PsA) is a painful autoimmune condition affecting millions worldwide. This debilitating disease not only causes joint inflammation and pain but is often accompanied by the skin condition known as psoriasis. Over the years, medical research has identified various types of PsA, each with different signs and symptoms. In this guide, we will explain the different types of psoriatic arthritis. Whether you are a newly diagnosed patient or a concerned caregiver, this article will help to expand your knowledge about the diverse presentations and management strategies related to PsA.
What is psoriatic arthritis?
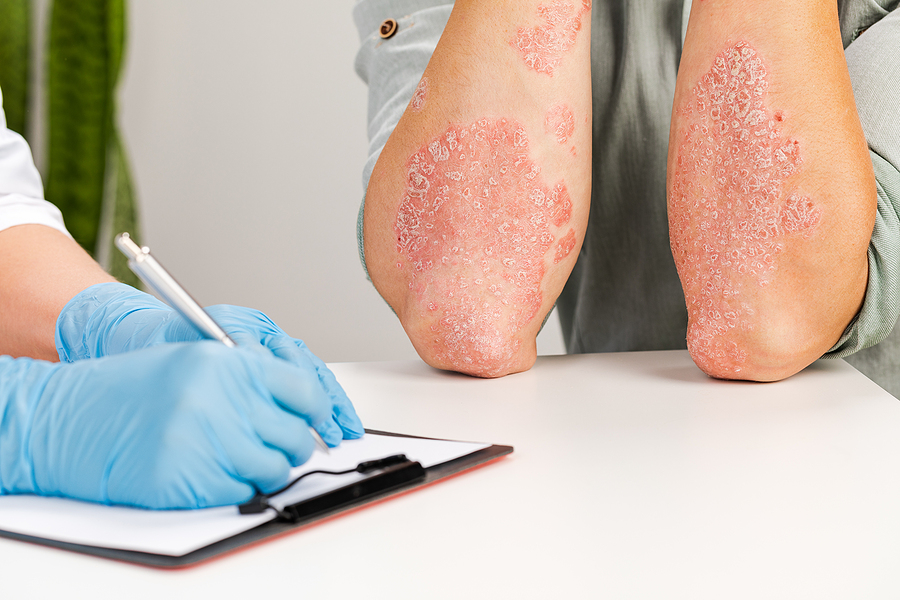
Psoriatic arthritis combines the symptoms of arthritis with the skin disorder psoriasis, which causes red, scaly patches to appear on the skin. PsA mostly affects the joints but can also involve the skin, nails, and sometimes the spine. Around 30% of people with psoriasis will develop PsA during their lifetime.
The most common signs and symptoms of psoriatic arthritis include joint pain, stiffness, swelling, and reduced range of motion. In some cases, psoriatic arthritis may also lead to fatigue, nail changes (such as pitting or separation from the nail bed), and eye inflammation.
What are the 5 types of psoriatic arthritis?
Understanding the five main types of PsA is crucial for accurate diagnosis and effective treatment. Let’s take a look at the five primary types of psoriatic arthritis:
1. Symmetric Arthritis: Symmetric arthritis is the most common type of PsA, affecting approximately 50% of people with the condition. These patients experience symmetric inflammation of joints on both sides of the body, such as the knees, wrists, and ankles. Swelling, pain, stiffness, and reduced range of motion are typical symptoms experienced by those with symmetric arthritis.
2. Asymmetric Arthritis: Asymmetric arthritis accounts for approximately 35% of PsA cases. Unlike symmetric arthritis, this subtype affects joints on one side of the body, or different joints on each side. It commonly involves the fingers, toes, knees, or ankles, and causes joint swelling, pain, and stiffness. Patients may also experience dactylitis; swollen, sausage-like digits.
3. Distal Interphalangeal Predominant: The distal interphalangeal predominant (DIP) subtype mostly affects the joints at the tips of fingers and toes. It causes joint inflammation, tenderness, and stiffness, often accompanied by nail changes, such as pitting or separation from the nail bed. This form of PsA can lead to progressive joint damage, resulting in impaired hand and foot function.
4. Spondylitis: Spondylitis is a type of PsA that mostly affects the spine and tailbone area, leading to pain, stiffness, and reduced mobility. Inflammation in these areas can cause discomfort in the neck, lower back, and buttocks. Those with spondylitis may experience morning stiffness and find it challenging to sit upright or perform daily activities.
5. Arthritis Mutilans: Arthritis mutilans is the rarest and most severe form of PsA. It causes rapid joint destruction, leading to severe deformities in the joints at the ends of the hands and feet.
How is psoriatic arthritis treated?
Psoriatic arthritis is treated differently depending on which subtype a patient is suffering from. Therefore, it’s extremely important that PsA is diagnosed properly, to allow for the development of a tailored treatment and management plan.
If you’re concerned about PsA, the rheumatology experts at Advanced Rheumatology of Houston can provide you with an accurate diagnosis and guide you through the best steps for managing your symptoms. Contact us here or call (281) 766-7886 to schedule some time with our rheumatology experts.